Hysterectomy does not help! Endometriosis and misconceptions about hysterectomy.
Why hysterectomy does not help?
Before I answer why hysterectomy does not help, I would like you to know what made me get to this conclusion.
Loving a woman with endometriosis can be very challenging, however, I’ve never abandoned my wife, even after realizing that we will never have kids. Furthermore, I learned how to support her.
I’m a husband behind a woman who suffers from multimorbidity, she has endometriosis and fibromyalgia.
Trying to help her research some information about the surgery she was about to go through, I noticed a lot of confusion behind endometriosis and hysterectomy.
My wife suffers from stage IV deep infiltrating endometriosis. It’s rare, only 1-5% of women affected by “endo” suffer from it.
She was about to go through her first surgery (a diagnostic laparoscopy), only to find during the procedure, how extensive her endometriosis was.
I decided to research what else could be done and found that hysterectomy does not help to cure endometriosis.
Here’s why…
Endometriosis is a condition that by definition exists outside of your uterus. It means, that neither a hysterectomy (removing the uterus), nor endometrial ablation (destroying the lining of the uterus), are correct treatments. Since there is no cure for endometriosis, and hysterectomy removes the uterus, not the endometrial tissue outside of it, hysterectomy does not help.
The truth is that ovaries cause the endometrium to grow outside the uterus, on other organs, and places in the pelvic area, so hysterectomy isn’t guaranteed to make the symptoms go away.
Additionally, key points to remember are the methods of hysterectomy, the long-term effects of it, and the recurrence of endometriosis after the procedure, what the surgery can and can’t do to relieve your pain, and if you have it done with or without oophorectomy.
The factors…
In order to understand why hysterectomy does not help women with endometriosis, we need to look at what hysterectomy is…
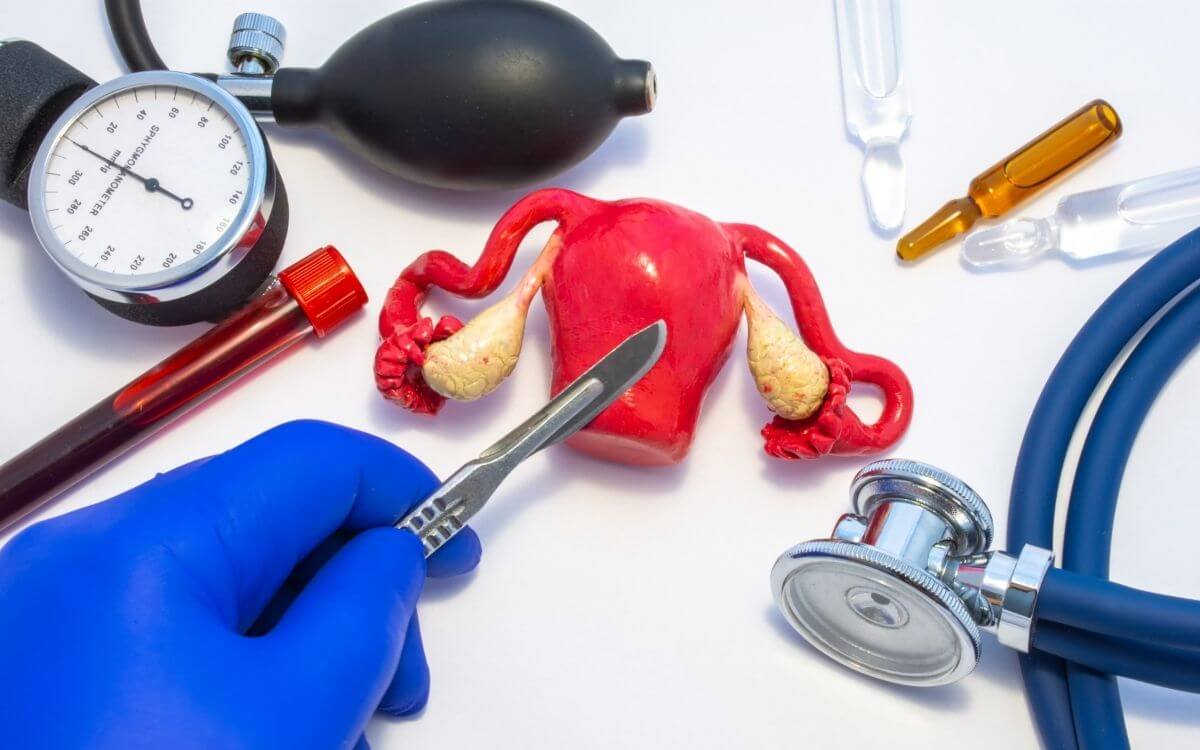
Hysterectomy is simply put a surgical removal of the uterus. Additionally, hysterectomy may involve removal of your cervix, ovaries, Fallopian tubes, and other surrounding structures.
Hysterectomy is usually performed by a gynecologist and may be total or partial. We’ll get to that later looking at the methods of hysterectomy.
Firstly, we need to look at all the factors behind this procedure, in order to give you more clarity about this life-changing decision that you may have once considered.
I decided to write this article because it shocked me how uninformed general practitioners are, and the last thing I want is for you to make the mistake of listening to someone’s bad advice.
You suffer enough. My heart goes to you! I’ve seen my wife crawl the walls because her pain was impossible to cope with.
She cannot take painkillers because they damage her stomach lining, giving a lot of gastric problems, including acid reflux and heartburn.
She is not able to take hormones either, they don’t suit her. Coil also wasn’t the option.
My wife has learned to combat her pain with mindfulness, breathing exercises, and light exercises such as pilates.
However, the possibility of reoccurrence of her endometriosis led me to research a little bit more about what could be done for my wife, in order to combat her brutal symptoms.
I found during my research of surgeries, that there is a lot of misconceptions about the disorder and hysterectomy, and that hysterectomy does not help endometriosis.
To give you more details, I’d like to invite you to read the following paragraphs. They will provide you with the answers to the following points:
- The methods of hysterectomy.
- The long-term effects of hysterectomy.
- The recurrence of endometriosis after the procedure.
- What the surgery can and can’t do to relieve your pain?
- Do you need a hysterectomy with or without an oophorectomy?
- Alternatives to hysterectomy.
The methods of hysterectomy.
They say that the hysterectomy is performed in three different ways – abdominally (TAH), vaginally (VH), and laparoscopically (LH), however, hysterectomy can be partial, complete, with the removal of ovaries, or radical.
Here are more details about the methods of hysterectomy:
- A partial (supracervical) hysterectomy involves the removal of the upper part of the uterus but leaves the cervix intact.
- A complete hysterectomy involves the removal of the uterus and cervix together.
- A hysterectomy with bilateral salpingo-oophorectomy involves the removal of the uterus, cervix, ovaries, and fallopian tubes.
- A radical hysterectomy involves the removal of all the reproductive organs, as well as the upper vagina, some lymph nodes, and surrounding tissue. This type of hysterectomy is usually performed when there is a cancer diagnosis.
The traditional hysterectomy is performed with an abdominal incision of about five inches It is done either – vertically or horizontally. The surgeon can easily see the uterus and surrounding area.
In a vaginal hysterectomy, a small internal incision will be made at the top of your genitals. A surgeon will separate the uterus from connecting tissue and its blood supply, after which will remove the uterus through the vaginal canal. The cervix may also be removed.
In a laparoscopic hysterectomy, small surgical tools will be inserted through two or three abdominal incisions, in order to remove the uterus in pieces. Your surgeon will control the laparoscopes with their robotic arms for extra precision.
Sometimes he will also use such a laparoscope during a vaginal hysterectomy, to get a better view of the uterus and surrounding organs.
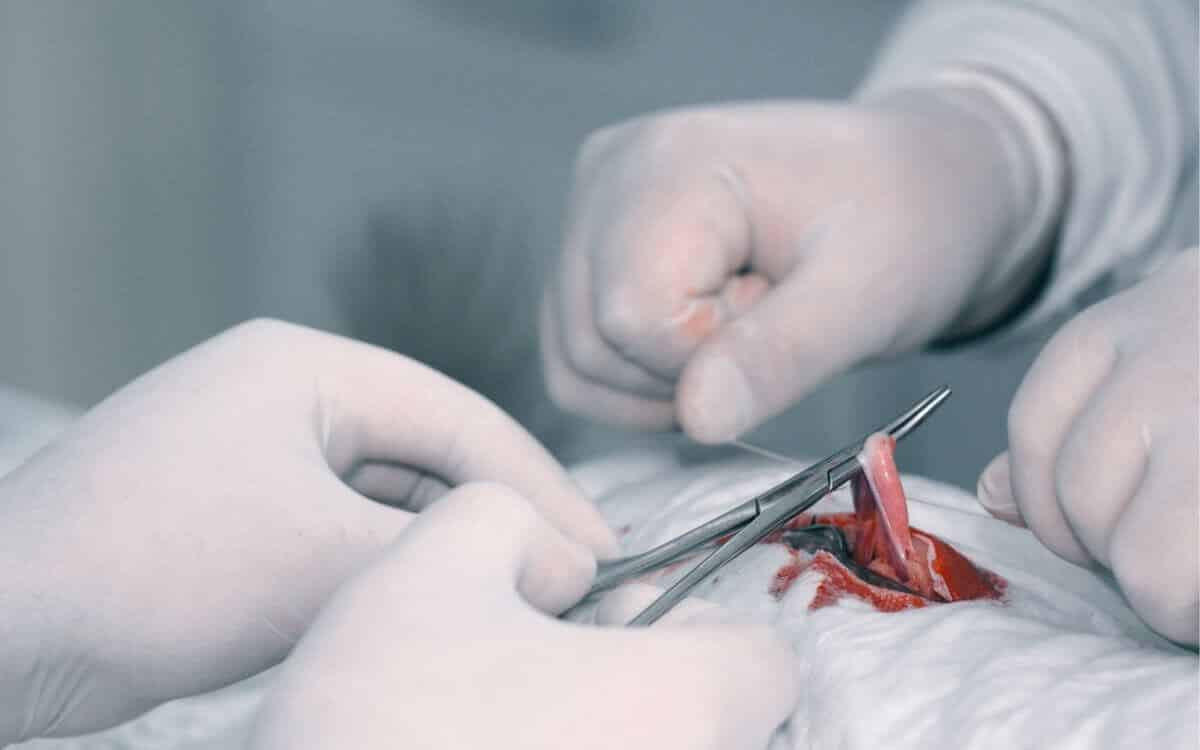
The long-term effects of hysterectomy.
There are plenty of disadvantages to having a hysterectomy in relation to your long-term health, especially if you didn’t have yet had natural menopause.
There are long-term effects of hysterectomy on the pelvic floor and you should consider surgical decision knowing that it may cause you to have the following:
- Pelvic organ prolapse.
- Urinary incontinence.
- Bowel dysfunction.
- Sexual function.
- Pelvic organ fistula formation.
If you decide to have a hysterectomy before the age of 40, there will be a higher risk of developing heart disease. If you have a hysterectomy with preservation of your ovaries before the age of 35, you may have an increased risk of congestive heart failure and risk of coronary heart disease.
Additionally, you may have a 13% increased risk of higher blood pressure and an 18% risk for obesity. Apart from that, two studies have suggested a significantly increased risk of dementia after surgical removal of the ovaries before their natural menopause.
We still have a lot to learn about the role that your uterus and ovaries play in interacting with other vital organs of your body and their contribution to your long-term health. So there are plenty of misconceptions about hysterectomy and endometriosis. So far, it goes to show that hysterectomy does not help women’s situation.
Women are being seriously affected by this procedure which adds many negative long-term effects. Hysterectomies are performed to improve quality of life, however, like any surgical procedure, it is generally associated with few complications.
The recurrence of endometriosis after the procedure…
Can endometriosis come back after hysterectomy? Yes, it can reoccur, and the hysterectomy will never guarantee you to cure your endometriosis.
Hysterectomy is one of the common treatments for endometriosis, however, it is reported that pain and other symptoms often reoccur. This is when a second operation is needed to remove endometrial implants that develop after the first operation in other parts of the pelvis.
The chance of reoccurrence of endometriosis after hysterectomy without removing your ovaries is as high as 62%… That’s terrible!
If you have a partial hysterectomy, leaving your cervix intact, it is possible that the symptoms of endometriosis will not go away after surgery.
Another surgical method is the removal of the ovaries (oophorectomy) during a hysterectomy. Studies show that this method has better results than just a hysterectomy, and fewer women need another surgery to treat endometrial implants. However, this method may cause premature menopause in young women.
The decision to have a hysterectomy has to be weighed by you beforehand. You need to take this into consideration because it will cause early menopause and impact your lifestyle.
The recurrence of your symptoms and pelvic pain are directly correlated to the precision of the surgery and removal of deeply infiltrated endometriosis. Your surgeon’s effort should always aim to remove the lesions completely, in order to keep the risk of recurrence of endometriosis as low as possible.
Bottom line is, it shows that hysterectomy does not help to cure endometriosis. There is more risk than benefits in my opinion. My wife never agreed to it.
Can you prevent endometriosis recurrence?
There are some options that you can take to prevent the recurrence of your endometriosis, but they include including hormonal treatment and diet modification.

Alternatives to hysterectomy.
After research that I would suggest you do you find that hysterectomy does not help endometriosis pain and symptoms to go away, you should consider alternatives to this procedure.
But what are they?
There are some alternatives, however, they might not be new to you if you’ve done your research.
I think I stressed it enough, that however desperate my wife was to treat her endometriosis pain, hysterectomy was never the first-line option for her.
M never takes painkillers, she never tried hormones either. Even after her 4-hour operation, to her surgeon’s surprise, she never took morphine! Instead, she learned to control her symptoms with her mind and a holistic approach with the following:
- Low Fodmap diet.
- Acupuncture.
- CBD balm to rub in the skin.
- Breathing exercises.
- Mindfulness and meditation.
- Avoidance of stress.
However, if you don’t agree with the holistic approach, you may consider other non-surgical alternatives or less invasive surgical procedures to directly treat endometriosis, such as:
- Over-the-counter pain like Advil (Ibuprofen).
- Oral contraceptives that can stop your period.
- Laparoscopy, to remove the excess of endo-tissue.
- Laparotomy, a traditional surgery, to remove the endometrial overgrowth.
- Surgery to sever the pelvic nerves in order to obtain pain relief.
All the above choices of treatment you should always consider based on the severity of your pain, your age, and your health, but also whether you have plans to have kids.
In July 2018, the F.D.A. approved Orilissa (Elagolix) as the first prescription drug used to treat endometriosis pain, however, I am not a fan of them as F.D.A. is business orientated.
They claim that taking it once or twice daily, Orilissa has proven effective in alleviating both menstrual and non-menstrual pelvic pain as well as pain during sex.
My conclusion…
In most cases, doctors will also start with conservative treatment such as medication before trying invasive surgical treatment, despite the fact that laparoscopy is the only way to diagnose endometriosis. In my opinion, medication is only good for acute pain, chronic pain has to be treated with a holistic approach.
My wife is the proof of that! We believe that hysterectomy does not help and that is always wise to try every single possible option before deciding to have this procedure.
The choice is always yours as every woman is unique and there is no one-fit-all solution. Good luck, I hope you found it helpful.
Take good care of yourself!

About Me
Hi, I’m Lucjan! The reason why I decided to create this blog was my beautiful wife, who experienced a lot of pain in life, but also the lack of information about endometriosis and fibromyalgia for men…
My experience….
I started my period at the age of nine, and had endometriosis pain from the very beginning. As I got older the worse the pain. Hormone therapy wasn’t available until my late teens. I found out very quickly that it was not an option for me. The hormones competed with mine own and caused a lot of complications. Nothing worked and I had to dull the pain with lost of medication. I dealt with it and managed my pain. I then tried having kids, which made everything worse. I miscarried 6 times. I finally had a baby boy. After the birth of my son, my endometriosis left me in pain all the time with only about 5 days of relief of pain a month. I finally had enough. I had a complete hysterectomy where they also removed my ovaries and fallopian tubes. I did that when I was 31 years old. I am now 45 and I do not regret my decision at all! I have no pain at all and I am finally so grateful that my pain is gone and my moods have stabilized. I feel amazing! A year ago I found out it saved me from having massive surgery on my heart because I had endometrium scaring in my heart valves. If it continued to grow it would have been much worse. I have never regretted my decision and have me a fell life for the first time!
Thanks for listening.
Thank you so much for sharing your story. I can’t begin to imagine the strength it took to endure all of that from such a young age. Starting your period at nine and dealing with endometriosis pain for so many years sounds incredibly difficult, and I’m so sorry you had to face the heartbreak of multiple miscarriages. The journey you’ve been on—the relentless pain, trying every option, and finally reaching a point where you chose a hysterectomy—is something that only someone who has experienced this can truly understand.
It’s really inspiring to hear that after everything, you’re finally pain-free and living life fully. I know that, for many women, the choice to have a hysterectomy is complex and often comes with fears and doubts. But hearing how it allowed you to reclaim your life and even prevented further complications is powerful. It reminds me of how important it is for everyone with endometriosis to have the freedom to make the choice that feels right for them.
Thank you again for sharing. Your strength and resilience are truly remarkable, and your story will no doubt give hope to others in similar situations.