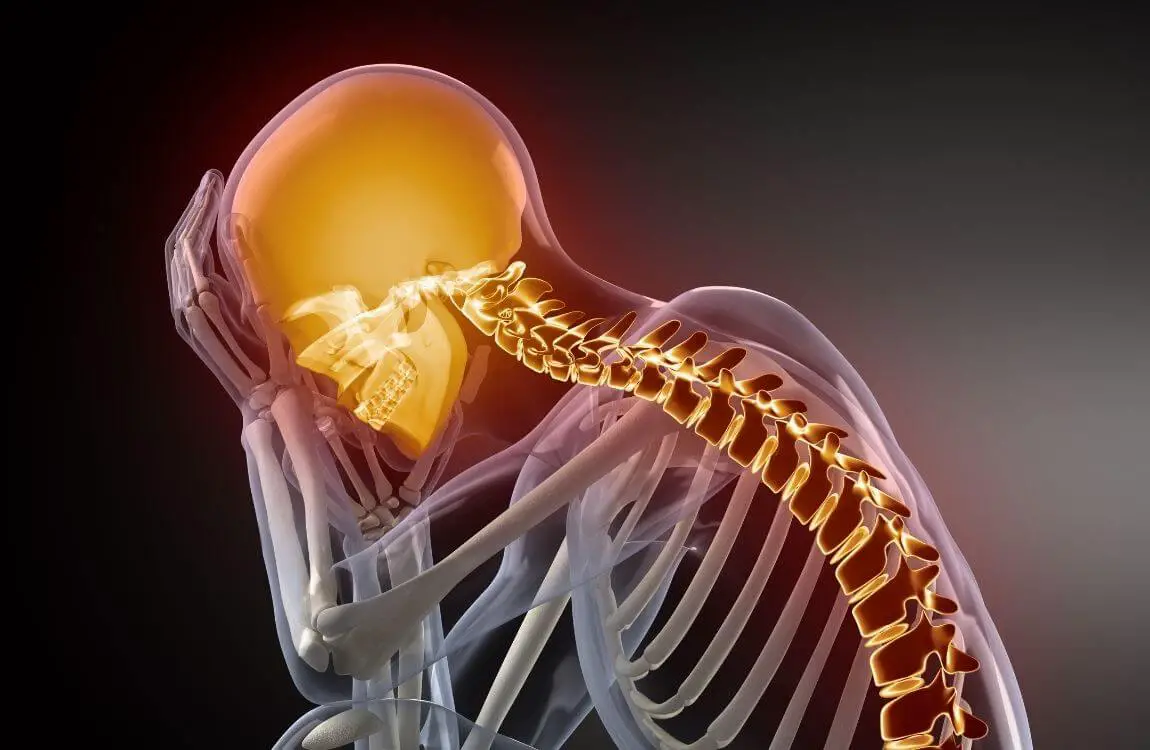
Challenges of living with multimorbidity, from a husband behind his chronically ill wife.
Challenges of living with multimorbidity…
Multimorbidity means that you have two or more long-term health conditions, which can include:
- Physical or mental health conditions, for example, endometriosis and anxiety.
- Ongoing conditions, such as learning disability.
- Complex symptoms, such as chronic pain.
- Sensory impairment, such as sight loss.
- Alcohol or substance misuse.
In this post, I discuss endometriosis and fibromyalgia because they affected my wife.
Not to mention that these chronic illnesses brought upon her severe OCD, general anxiety, panic disorder, and depression with suicidal feelings.
It also affected me as her primary support.
That’s complex! These are the real challenges of living with multimorbidity.
Multimorbidity is associated with:
- Reduced quality of your life.
- In some cases, reduced life expectancy.
- Repetitive treatment.
- Mental health impact.
- Functional difficulties.
- Increased use of health services.
- Increased use of medication.
The challenges of living with multimorbidity also include:
- Difficulties in the management of your illness.
- Struggles with day-to-day activities.
- A need to receive care from multiple services.
- It affects your mental, emotional and psychological health.
- Frequent and unplanned emergency care.
- Having side effects of the medication you may have to take.
Just as multiple health problems create difficulties for the sufferer, they also create problems for partners who support them:
- Caregiving partners deal with uncertainty and confusion not knowing what to do.
- Disagreements between the couple often occur.
- Caregivers are often forgotten.
- They feel worried about their spouse.
- They become sole breadwinners.

The challenges…
Multimorbidity is challenging not only for the person who sufferer from multiple chronic conditions but also for the partner with who they live.
So in order to manage partners’ chronic illnesses better, caregivers need to educate themselves about it.
Women with endometriosis are more likely to have other chronic conditions, such as:
- Fibromyalgia
- Chronic fatigue syndrome
- Autoimmune disorders
- Allergies, asthma, and eczema
- Endocrine disorders
In regards to fibromyalgia, women with endometriosis are twice as likely to have it as those who don’t have endometriosis.
My wife developed fibromyalgia after her laparoscopy. The trauma of being diagnosed with one untreatable condition brought upon her another.
My wife was diagnosed with the most severe form of endometriosis (stage 4), called deep infiltrating endometriosis.
This stage consists of multiple deep implants, large cysts on one or both ovaries, and thick adhesions, reaching the bowel.
Most women with endometriosis get pain in the area of their hips and legs but it isn’t uncommon for this pain to spread to the upper body.
For women who experience such pain all the time, exhaustion and tiredness are common.
Adding to endometriosis the complexity of widespread pain from fibromyalgia makes trying to be okay a full-time job.
The challenges of living with multimorbidity are vast.
Men also struggle. An example of that would be managing the variety of new tasks which fall upon them, they must become:
- Caregivers
- Cleaners
- Cooks
- Nurses
- Advocates
- Sole breadwinners
It’s hard for both parties. Some men fail to adopt and leave their women.
The endometriosis divorce rate is higher than of the healthy couples or couples where fibromyalgia is present.
The reason for it is that for women with endometriosis having sex can be extremely painful.
This makes them feel guilty for refusing sex with their partners.
At the same time, men feel rejected and frustrated, although oftentimes they restrain themselves from having sex in fear of hurting their partners.
One of the other challenges of living with multimorbidity is a lack of sleep.
Chronic pain can interfere with sleep, leaving both partners tired, fed up, irritated. This may lead to arguments.
Not being able to work, life becomes more difficult and you begin to think about how to make money when you have a chronic illness.

Anxious times!
Throughout the years, my wife and I have learned several coping mechanisms that keep our marriage healthy.
Instead of going against each other, we support one another in the most difficult times.
You mustn’t forget that just because you are her primary caregiver, you will have moments of doubt, and this is when you will need her most.
It will surprise you how vast the challenges of living with multimorbidity are. One of the most obvious things you’ll notice is how it impacts your mental health.
Anxiety – it is worrying about the future that you cannot predict. No matter how much you try, you can’t, you won’t.
Chronic illness causes extreme anxiety because the ill partner cannot predict what tomorrow is going to bring.
But even though they have no evidence of something happening in the future, they believe in it so strongly, it’s difficult to change their anxious mind.
Depression – it’s an outcome of overthinking. It’s similar to anxiety, but a depressed person thinks of the past.
“Why are you with me?” – my wife asked many times.
“I love you, and I will never leave you, despite what you think of yourself. You’re still the same person I’ve met, even though you can’t see it. Falling ill isn’t your fault.” – I said.
She even asked me on three separate occasions to divorce her for the sake of my happiness.
But I never said I wasn’t happy! Sure, occasional disagreements happen, but which relationship doesn’t go through it?
In some strange way, the challenges of living with multimorbidity brought us closer together.
Our intimacy is on a such deep level, I couldn’t achieve that with a healthy woman. “Why,” – you ask?
Because chronic illness makes you extremely vulnerable every couple eventually reaches the point where they have to be completely honest with each other.
They express how they feel, what worries them, what are they afraid of, and what can be done to improve their relationship.
In order for their relationship to work, they need to communicate. Such communication is on another level.
They cannot hide what they feel. That brings them closer, they have no secrets, they both are like an open book.
Adjustment.
One of the best tips I can give to all men caring for their women with multiple chronic illnesses is, that you can’t control it.
You cannot fix her chronic illness, you have to work on adjusting yourself to the new situation.
You have to put in some work I’m afraid, no one said it was easy. But it will pay off in the long run.
You must remember that for her, just staying well is a full-time job. You’re healthy, you’re mobile, the world is your oyster. You shouldn’t complain.
A bit of adjustment won’t hurt.
“Why bother at all” you may ask if you can have a better life with someone else?
Remind yourself what made you want her. What was that gave you these butterflies? Find it, follow it, remind yourself of these good things in her that you love so much!
Just because she has chronic illnesses doesn’t mean your life is over.
Both of you must learn to recognize how you’re feeling and how to express it to each other. You really have to learn proper listening in a non-judgmental way.
Sometimes you may get so distressed and it’s difficult to manage your emotions, which can lead to a distance between you.
But practice makes perfect!
You both need to work to educate one another, share research, articles, and books on living with chronic illness.
In my case, it is endometriosis and fibromyalgia that I constantly educate myself about. But M gives me articles she discovers.
If you don’t know where to start, the fest practice is to make some notes on what your limitations, boundaries, and triggers are.
Keeping such a journal allows you to plan ahead.
For instance, my wife knows a few months ahead when will she roughly be on her period or/and go through ovulation.
Whenever we want to go away for a holiday, we plan it around her period and ovulation calendar.
Cramps with ovulation and painful periods can really ruin her holiday, so she plans our holiday between ovulation and period. We usually have a two-week window.
Such planning makes life easier.

The awareness of multimorbility.
I decided to take an interest in the challenges of living with multimorbidity because I noticed a lack of awareness of it.
Especially of endometriosis and fibromyalgia together.
Women with endometriosis aren’t taken seriously as much as people with fibromyalgia.
Endometriosis isn’t widely known as fibromyalgia is. That creates additional problems with the experience of pain.
It can be difficult to pinpoint if you suffer from endometriosis or fibromyalgia flare-up. They often overlap, causing worse pain experiences.
Medicine is focused on helping people with acute pain (like a broken leg or an injury) rather than the management of long-term conditions.
Even if classical medicine focuses on long-term conditions, they often think of diabetes, obesity, or heart failure.
Most of them are in most cases self-induced with a bad diet, lack of exercise, and an overall unhealthy lifestyle.
This isn’t fair because people who develop endometriosis or fibromyalgia aren’t in control, it isn’t up to them, they did not choose to have these illnesses.
And yet, they are more marginalized than people who inflicted on themselves their own health problems.
Additionally, classic medicine doesn’t promote holistic coordinated care for people with multiple conditions.
And what makes things worse, they promote drugs over a holistic approach to care because it brings them money.
Even though the challenges of living with multimorbidity become more common, doctors choose shortcuts in the form of pills rather than natural treatment.
Providing holistic care for chronic diseases is inconvenient, inefficient, and unsatisfactory, both for most doctors.
That leads people with multimorbidity to treatment decisions that are inappropriate and in some cases unnecessary.
Doctors don’t treat anyone these days looking at them as a whole person but like a number that fits or doesn’t fit the system.
People with multimorbidity have worse quality of life, increased rates of anxiety and depression but they are seen as worry heads.
You probably went through the same process as my wife did. Doctors kept telling M that it was all in her head.
They tried to prescribe antidepressants saying that her symptoms were due to anxiety, when in fact, it’s the symptoms of endometriosis and fibromyalgia that caused her distress.
Such mistreatment is so common, it doesn’t give sufferers much confidence in general practitioners. All that delays their diagnosis.
Years are wasted, and the symptoms of illnesses like endometriosis and fibromyalgia progress.
Such negligence and utter disbelief in my wife’s invisible symptoms caused her to develop the worst stage 4 deep infiltrating endometriosis.
Conclusions…
Living with one disease is hard enough, living with multiple chronic illnesses and staying sane is a full-time job.
But chronic illnesses such as endometriosis and fibromyalgia cause chronic pain and impact mental wellness.
The challenges of living with multimorbidity affect not only the person who suffer but their partners, family, their financial and social situation.
There are many worries that come to mind, but open communication, support, spreading awareness, and advocacy, however hard, make life worthwhile.
To finish off, I’d like to give you more tips to cope when you’re juggling several chronic illnesses, especially endometriosis and fibromyalgia…
If you’re alone, be proactive in your own health care with these strategies. Because if you don’t take care of yourself no one will.
Unless you have a supportive partner…
So, if you’re the one who supports his loved one:
Get educated about her conditions.
Talk with her doctor about what you can do. But not only that, pelvic floor therapists, physiotherapists or nutritionists, and other professionals specializing in chronic health conditions.
They can help to advise her on how to exercise or how to eat a healthy specific for endometriosis and fibromyalgia diet.
It will help her take control of the conditions she already has and to prevent conditions she worries about getting.
Become an expert in medication.
Find out what each of her medications does, why she needs it, what side effects you should particularly watch for, and how it may interact with other drugs.
Don’t rely solely on the internet, it’s safer if you get such information from a pharmacist.
Accompany her if she visits many doctors, be sure each of them knows what medicines the other doctors have prescribed and that they follow each other.
Take notes. Again, this is where having a journal comes in handy! (You need to have some electronic health records in case they screw things up, as believe me, hospital records do get lost).
Journaling is a great way to keep track of her symptoms and treatments. If she’s having symptoms you think may be side effects of a medicine or an adverse interaction between drugs, use your journal to record when you take medications, when symptoms develop, and how long the symptoms last.
Be her private advocate.
Remember that no one understands how she’s feeling better than her.
Ask her questions and don’t be afraid to speak up for her if she’s having trouble managing her conditions or if she’s concerned about the way doctors are doing their job.
Be there for one another. Love each other, never lose hope. Keep moving forward.
Winston Churchill once said: “if you’re going through hell, keep going”! Eventually, things get better.
All the best!

About Me
Hi, I’m Lucjan! The reason why I decided to create this blog was my beautiful wife, who experienced a lot of pain in life, but also the lack of information about endometriosis and fibromyalgia for men…